Understanding
Congenital Heart Defects
Expert information about ASD, VSD, PDA, Tetralogy of Fallot, and Coarctation of the Aorta
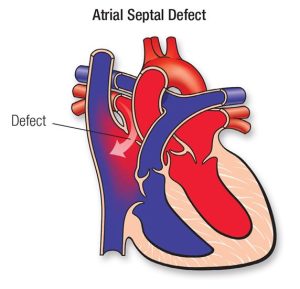
Atrial Septal Defect
What It Is?
An atrial septal defect is a hole in the wall (septum) that separates the heart’s two upper chambers (the left and right atria). This opening allows oxygen-rich blood from the left atrium to leak into the right atrium, where it mixes with oxygen-poor blood.
What Happens Because of this extra blood flow, the right side of the heart and the lungs must work harder. The right heart chambers may enlarge over time as they handle the increased volume.
Signs and Symptoms Many children with small ASDs have no symptoms. Larger defects may cause:
- Fatigue during feeding or play
- Frequent respiratory infections
- Shortness of breath
- Heart murmur detected during checkup
Treatment Options
- Small ASDs: May close on their own during the first few years of life; regular monitoring with your cardiologist
- Medium to Large ASDs: Can often be closed with a catheter-based device inserted through a vein (no open-heart surgery required)
- Very Large or Complex ASDs: May require open-heart surgery to place a patch
Long-Term Outlook When treated appropriately, children with ASD typically do very well. Untreated large ASDs can lead to heart failure, stroke risk, and pulmonary hypertension in adulthood, which is why regular cardiology follow-up is essential.
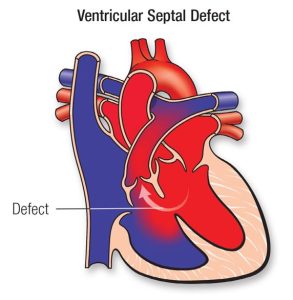
Ventricular Septal Defect
What It Is?
A ventricular septal defect is a hole in the wall separating the heart’s two lower chambers (the left and right ventricles). This is the most common type of congenital heart defect.
What Happens
High-pressure, oxygen-rich blood from the left ventricle flows through the hole into the right ventricle, mixing with oxygen-poor blood. This forces the left side of the heart to pump harder, and the lungs receive more blood than they should.
Signs and Symptoms
- Fast breathing or breathlessness during feeding
- Poor weight gain or failure to thrive
- Sweating during meals
- Frequent lung infections
- Heart murmur (often the first sign noticed by your pediatrician)
Treatment Options
- Small VSDs (Restrictive): About half close on their own by age 2; others may remain small and harmless with yearly checkups
- Moderate VSDs: May require medication to help the heart work more efficiently while monitoring for spontaneous closure
- Large VSDs: Typically require surgical patching within the first 3-6 months of life to prevent lung damage
Long-Term Outlook After successful repair, most children lead completely normal, active lives. Large uncorrected VSDs can lead to irreversible lung disease (Eisenmenger syndrome), which is why timely treatment is crucial.
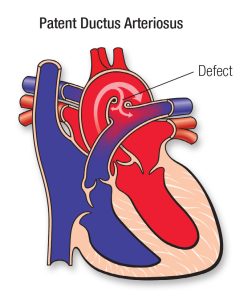
Patent Ductus Arteriosus
What It Is?
Before birth, all babies have a blood vessel called the ductus arteriosus that connects the pulmonary artery to the aorta, allowing blood to bypass the lungs (which aren’t yet breathing). This vessel normally closes within the first few days after birth. When it stays open, it’s called a patent ductus arteriosus.
What Happens
Blood that should flow to the body instead recycles back to the lungs, causing the lungs and the left side of the heart to become overloaded with extra blood flow.
Signs and Symptoms
- Rapid breathing or breathlessness
- Poor feeding and slow weight gain
- Sweating during feeding
- Continuous “machinery-like” heart murmur
- More common in premature infants
Treatment Options
- Premature Infants: Medication (indomethacin or ibuprofen) given through an IV can often close the PDA
- Older Infants and Children: Catheter-based closure using a small coil or occluder device (outpatient procedure)
- Surgical Closure: Reserved for very small premature babies or cases where catheter closure isn’t possible
Long-Term Outlook Once closed, the PDA typically causes no further problems. Untreated large PDAs can lead to heart failure, pulmonary hypertension, and increased risk of endocarditis (heart infection).
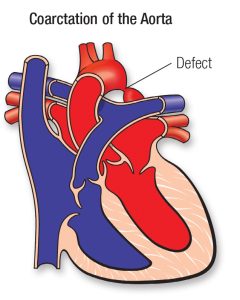
Coarcation of the Aorta
What It Is?
Coarctation of the aorta is a narrowing of the body’s main artery (the aorta), typically located just past where the blood vessels to the head and arms branch off. Think of it as a pinch or kink in a garden hose.
What Happens
The heart must work much harder to push blood past the narrowed section. This causes high blood pressure in the upper body (arms and head) while the lower body (legs) receives less blood flow with weaker pulses.
Signs and Symptoms
In Newborns:
- May appear completely healthy at first
- Sudden collapse or shock when the ductus arteriosus closes (usually within first week)
- Difficulty breathing
- Poor feeding
- Cool or pale legs
In Older Children:
- High blood pressure in the arms
- Weak or absent pulses in the legs
- Cold feet
- Leg cramps or pain with exercise
- Headaches or nosebleeds
- Often discovered during a routine sports physical
Treatment Options
- Severe Cases in Newborns: Emergency medication (prostaglandin) to reopen the ductus arteriosus and restore blood flow to the lower body until surgery
- Surgical Repair: Removing the narrowed section and reconnecting the aorta, or widening it with a patch
- Balloon Angioplasty: Inflating a balloon inside the narrowed area; may also include placing a stent (expandable metal tube)
- Timing depends on severity – critical cases need repair within days; milder cases can be scheduled electively
Long-Term Outlook
Most children recover well from coarctation repair. However, lifetime surveillance is necessary to monitor for re-narrowing, aneurysm formation at the repair site, and persistent high blood pressure. Regular cardiology and sometimes blood pressure medication are part of long-term care.
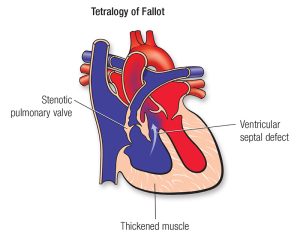
Tetralogy of Fallot
What It Is?
Tetralogy of Fallot is the most common cyanotic (blue-baby) heart defect. It’s actually a combination of four problems occurring together:
- A large ventricular septal defect (VSD)
- Pulmonary stenosis (narrowing of the valve and artery leading to the lungs)
- Right ventricular hypertrophy (thickened heart muscle)
- An overriding aorta (the main artery “straddles” both ventricles instead of connecting only to the left)
What Happens
Because of the pulmonary stenosis, not enough blood reaches the lungs to pick up oxygen. Oxygen-poor blood crosses through the VSD and flows directly to the body through the overriding aorta. This causes low oxygen levels in the blood, giving babies a bluish tint (cyanosis).
Signs and Symptoms
- Blue or purple coloring of lips, tongue, and skin (especially during crying or feeding)
- Rapid breathing
- Poor weight gain
- Clubbing of fingers and toes (in older unrepaired children)
- “Tet spells” – sudden episodes of severe cyanosis and breathlessness, often relieved when the baby squats or pulls knees to chest
Treatment Options
Tetralogy of Fallot always requires open-heart surgery, typically performed between 3-6 months of age. The surgery involves:
- Closing the VSD with a patch
- Opening up or widening the narrowed pulmonary valve and artery
- Sometimes placing a temporary shunt in very small or premature babies, with complete repair at a few months old
Long-Term Outlook
Most children do extremely well after TOF repair and lead active, normal lives. However, lifelong cardiology follow-up is necessary because some patients need a pulmonary valve replacement during adolescence or adulthood due to valve leakage.
_“Content courtesy of (MedicalCentric and iHeartChangeProgram). Used for informational purposes only.”_
